What is High blood pressure?
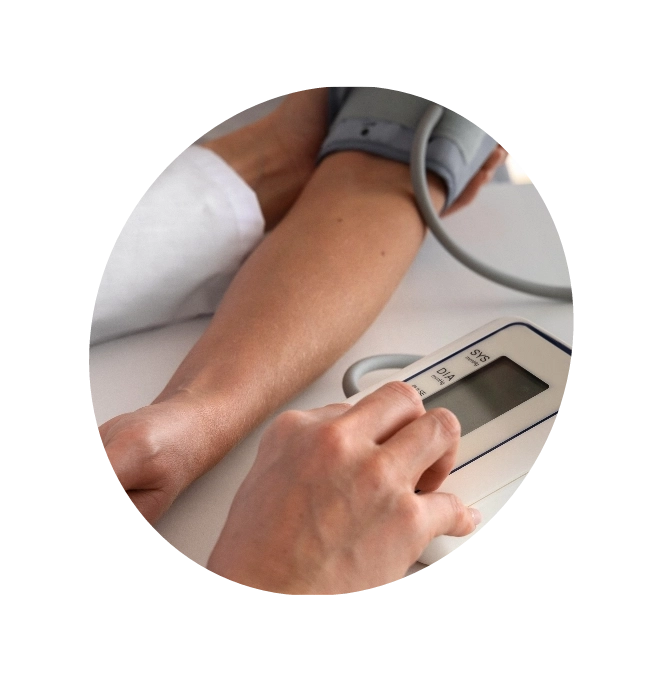
Hypertension is often referred to as the ‘silent killer’ because it does not show any visible signs until it reaches dangerously high levels. If left untreated, this condition can lead to considerable organ damage but can be prevented with the right treatment. Hypertension is a serious medical condition in which the pressure applied by flowing blood on the walls of arteries is too strong. Your blood pressure measurement consists of two numbers: systolic and diastolic.
Systolic measurement
Systolic measurement is the pressure of blood against your artery walls when the heart has just finished pumping (contracting). The top number, or systolic measurement, of a blood pressure reading.
Diastolic measurement
Diastolic measurement is the pressure of blood against your artery walls between heartbeats when the heart is relaxed and filling with blood. The second value in a blood pressure reading
Level
Systolic
Diastolic
High blood pressure is:
140 or above
90 or above
Prehypertension is:
120 to 139
80 to 89
Normal adult (age 18 or older) blood pressure is:
119 or below
79 or below
According to new, more stringent high blood pressure guidelines from the Seventh Report of the Joint National Committee (JNC 7) on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure, millions of people with previously considered borderline high (130 to 139/85 to 89 mm Hg) or normal (120/80) blood pressure now fall into the “prehypertension” range.
Because new studies show the risk of heart disease and stroke begins to increase at lower blood pressures than previously believed, health experts lowered the acceptable normal range to promote more aggressive and earlier treatment of high blood pressure.
Symptoms of High Blood Pressure
Usually, you will not feel any warning signs or high blood pressure symptoms, and you will not know you have it until a health professional takes a reading. Hypertension develops slowly and can cause serious organ damage, usually without any symptoms.
If you develop severe high blood pressure, you may have headaches, visual disturbances, nausea, and vomiting.
Malignant high blood pressure which is hypertension that rises rapidly, can also cause similar symptoms. Untreated malignant hypertension can damage the brain, heart, eyes, or kidneys. It is a medical emergency that requires immediate hospitalization.
Over time, if you do not receive treatment for this condition, you may experience symptoms caused by damage to your heart, kidney, or eyes, including coronary artery disease, stroke, and kidney (renal) failure.
Hypertension Causes
It is not always easy for a doctor to determine the root cause of hypertension, Factors such as obesity, heavy alcohol consumption, genetic predisposition to high blood pressure, high salt intake and advancing age can all contribute to raising one’s blood pressure. In addition to sedentary habits, stress and less than sufficient potassium or calcium in your diet, insulin resistance can also lead to elevated blood pressure.
Several factors increase your risk for high blood pressure. Some of them are lifestyle issues you can control. Lifestyle issues you can control to lower your risk of developing high blood pressure include obesity and not being active or exercising, drinking alcohol (three drinks a day or more), eating a lot of salty or processed foods, and not getting enough calcium, magnesium, and potassium in your diet.
Risk factors you can’t control include a family history of high blood pressure, your race (being African American increases your risk), and aging. Ninety percent of people who, at age 55, do not have hypertension will eventually develop it.
How is High Blood Pressure Diagnosed?
During routine doctor visits, many individuals come to realize that they have high blood pressure. To confirm that you have high blood pressure, your blood pressure must reach or exceed 140/90 mm Hg on three or more separate occasions. It is usually measured in intervals of 1-2 weeks. Except in very severe cases, the diagnosis is not based on a single measurement.
If there is a reason to suspect that the blood pressure measurements taken in the doctor’s office do not represent your accurate blood pressure (if, for example, you have white-coat hypertension), you may need to check your blood pressure away from the doctor’s office. Your blood pressure can rise more than 20 mm Hg systolic and 10 mm Hg diastolic from white-coat hypertension. Even routine activities, such as attending a meeting, can raise your blood pressure by that amount. Other factors that can raise your blood pressure include commuting to work, exposure to cold, and drinking large amounts of alcohol.
Your doctor may have you check your blood pressure at home 3 times a day and keep a record of the readings. Or you may need to wear an automated blood pressure cuff that periodically inflates and takes blood pressure measurements during the day. This is called ambulatory blood pressure monitoring.
Asthma Treatment
If you fall into the prehypertension range (120-139/80-89 mm Hg), your doctor will likely recommend lifestyle modifications, including losing excess weight, exercising, limiting alcohol, cutting back on salt, quitting smoking, and following the Dietary Approaches to Stop Hypertension (DASH) diet. The DASH eating plan is a low-fat and low-saturated-fat diet that emphasizes eating more fruits, vegetables, whole grains, and low-fat dairy foods.
If you have high blood pressure (140-159/90-99 mm Hg) and you do not have any organ damage or other risk factors for heart disease (uncomplicated high blood pressure), your doctor may suggest lifestyle changes and/or medicines to help manage it. Most people with high blood pressure will need two or more medications, including a thiazide-type diuretic, to lower their blood pressure to below 140/90 mm Hg, the goal for people with uncomplicated hypertension. If you have other conditions, such as diabetes, heart failure, or chronic kidney disease, your goal blood pressure is lower: 130/80 mm Hg.
If your blood pressure is 160-179/100-109 mm Hg or higher, you and your doctor may need to try various combinations of medications to find what works best for you. You will also need to make aggressive lifestyle changes.
Overall, your treatment will depend upon how high your blood pressure is, whether you have other medical conditions, such as diabetes, and whether any organs have already been damaged. Your risk of developing other diseases, especially heart disease, will be another important factor your doctor will consider.
Deciding whether to treat high blood pressure with medication and choosing the best medication are based mainly on:
- Your blood pressure measurement.
- Whether there are signs of organ damage caused by high blood pressure in other parts of your body, such as an enlarged heart or early damage to your arteries, kidneys, or eyes.
- Whether you have other medical conditions, such as heart disease, diabetes, or kidney or lung disease, or risk factors for heart disease, such as diabetes or high cholesterol.
- Whether you think you can be successful in making lifestyle changes.
Doctors may have different opinions about when to start medications for high blood pressure.
- If you have prehypertension (120-139/ 80-89 mm Hg) or high blood pressure (140/90 mm Hg), you do not have other risk factors for heart disease, and there’s no evidence of organ damage, lifestyle changes alone may be tried before medication.
- If you have other risk factors for heart disease, there is evidence of damage to organs, or you have stage 1 or 2 high blood pressure, treatment with medication is often started in addition to lifestyle changes.
Doctors usually prescribe a single, low-dose medication first. If blood pressure is not controlled, he or she may change the dosage or try a different medication or combination of medications. It is common to try several medications before your blood pressure is successfully controlled.
Many people need more than one medication to get the best results.
Medication Choices
Medication choices include: Diuretics. Hydrochlorothiazide- Furosemide- Spironolactone
Beta-blockers:
- Sectral
- Acebutolol
- Coreg
- Carvedilol
- Tenormin
- Atenolol
- Kerlone
- Betaxolol
- Normodyne, Trandate
- Labetalol
- Lopressor, Toprol XL
- Metoprolol
- Corgard
- Nadolol
- Levatol
- Penbutolol
- Visken
- Pindolol
- Inderal
- Propranolol
- Blocadren
- Timolol
ACE inhibitors:
- Lotensin
- Benazepril
- Capoten
- Captopril
- Vasotec
- Enalapril
- Monopril
- Fosinopril
- Prinivil, Zestril
- Lisinopril
- Mavik
- Trandolapril
- Accupril
- Quinapril
- Altace
- Ramipril
- Aceon
- Perindopril
Calcium channel blockers.
- Cardizem SR, Dilacor XR, Tiazac
- Diltiazem
- DynaCirc
- Isradipine
- Cardene
- Nicardipine
- Adalat, Procardia XL
- Nifedipine
- Sular
- Nisoldipine
- Calan SR, Isoptin SR
- Verapamil
- Norvasc
- Amlodipine
- Lotrel
- AmlodipineAmlodipine and benazepril hydrochloride
- Plendil
- Felodipine
- Lexxel
- Enalapril maleate-felodipine ER
Angiotensin II receptor blockers (ARBs).
- Cozaar, Hyzaar
- Losartan
- Diovan
- Valsartan
- Avapro
- Irbesartan
- Atacand
- Vandesartan cilexetil
- Benicar
- Olmesartan
- Teveten
- Eprosartan mesylate
- Micardis
- Telmisartan
All these medications are effective for lowering the risk of heart attack and stroke. Treatment for high blood pressure must be highly individualized and based on your risk factors, such as diabetes, smoking, and heart disease. Although one study may recommend a particular medication as the first line of treatment, it may not be best for you based on your medical condition. What’s most important is that you work with your doctor to find the right medication or combination of medications that have the fewest side effects and work well for you and that you take your medications regularly as prescribed.
New high blood pressure guidelines from the Seventh Report of the Joint National Committee (JNC 7) on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure recommend that, for most people, one of the medications be a thiazide-type diuretic.
If other conditions, such as heart failure or diabetes, are present, ACE inhibitors or ARBs often are used as the first line of therapy because the other medical conditions also may benefit from these medications. However, isolated systolic hypertension may respond best to diuretics alone.
If the above medications are not effective in lowering blood pressure, or if side effects of the above medications are serious, other medications called vasodilators may be tried.
What to think about
- Experts recommend using calcium channel blockers and/or ACE inhibitors only if diuretics and beta-blockers fail to control blood pressure and if certain other risk factors are present. For example, a type of calcium channel blocker works well in older people with isolated systolic hypertension. ACE inhibitors are often prescribed if you have heart failure or diabetes as well as high blood pressure.
- Some people who develop a cough while taking ACE inhibitors do well with ARBs, which usually do not cause a cough.
- Strategies for treating high blood pressure in pregnant women are quite different. For more information, see the topic of Preeclampsia and Hypertension During Pregnancy.
- Some experts believe a combination of medications, each given in a lower dose, is better for reducing blood pressure than a higher dose of a single medication. Because the medications that are combined are given in a lower dose, there are fewer side effects from the drugs.