Prostate Cancer
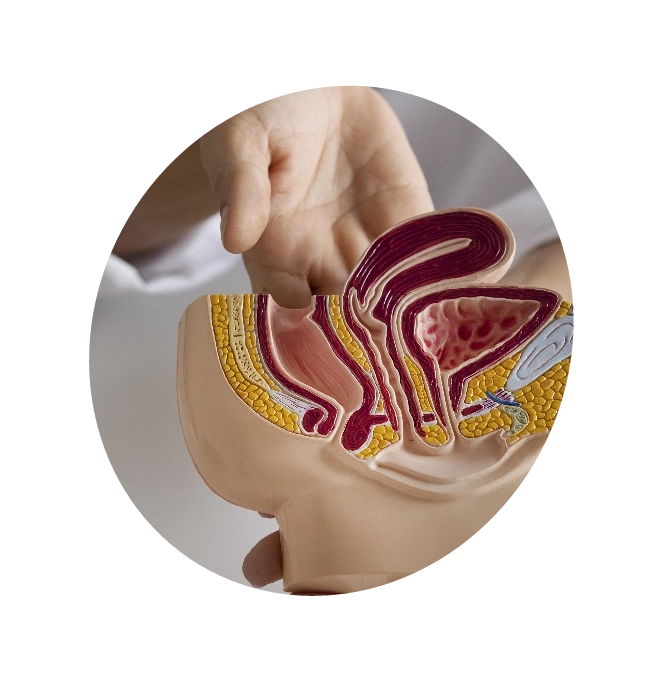
Prostate cancer is cancer of the prostate gland. This is the small, walnut-shaped gland that surrounds the bottom portion (“neck”) of a male’s bladder and about the first inch of the urinary tube (urethra), the channel that drains fluid from the bladder.
What is Prostate Cancer?
For many men, a diagnosis of prostate cancer can be frightening not only because of the threat to their lives but because of the threat to their sexuality. The possible consequences of treatment which include bladder control problems and erectile dysfunction (ED) or impotence can be a great concern for some men.
Prostate cancer is cancer of the prostate gland. This is the small, walnut-shaped gland that surrounds the bottom portion (“neck”) of a male’s bladder and about the first inch of the urinary tube (urethra), the channel that drains fluid from the bladder. It’s located behind the pubic bone and in front of the rectum. The prostate’s primary function is to produce seminal fluid, the fluid that nourishes and transports sperm.
This type of cancer is the most common cancer in American men. The American Cancer Society estimates that about 230,000 men are diagnosed with prostate cancer annually in the United States and that about 29,000 men die of the disease.
Detecting prostate cancer early when it is still confined to the prostate gland improves your chances for successful treatment. Successful treatment of cancer that has spread beyond the prostate gland is more difficult. But treatments exist that can help control cancer.
Signs and Symptoms of Prostate Cancer
Prostate cancer often doesn’t produce any symptoms in its early stages. It is because of this that most cases of prostate cancer go undetected until they have spread beyond the prostate.
When signs and symptoms do occur, they may include the following:
- Dull Pain in Your Lower Pelvic Area
- Urgency of Urination
- Difficulty Starting Urination
- Pain During Urination
- Weak Urine Flow and Dribbling
- Intermittent Urine Flow
- a Sensation That Your Bladder Isn’t Empty
- Frequent Urination at Night
- Blood in Your Urine
- Painful Ejaculation
- General Pain in Your Lower Back, Hips, or Upper Thighs
- Loss of Appetite and Weight
- Persistent Bone Pain
Popular Prostate Cancer Medications
Emend Tri Pack
Starting from:
$195.00
Orgovyx
Starting from:
$410.00
Nolvadex D
Starting from:
$40.00
Lupron Depot Kit
Starting from:
$225.00