Complementary and alternative therapies for pain and stress management aren’t new. Meditation and yoga are two ancient forms of practice that have been around for millennia. Nevertheless, their use has been on the rise lately, predominantly among people suffering from chronic illnesses like fibromyalgia.
Several of these treatments do appear to safely relieve stress and reduce pain, and some are gaining acceptance in mainstream medicine. But many practices remain unproved because they haven’t been adequately studied.
Some of the more common complementary and alternative treatments promoted for pain management, and the current thinking about their effectiveness and safety, include:
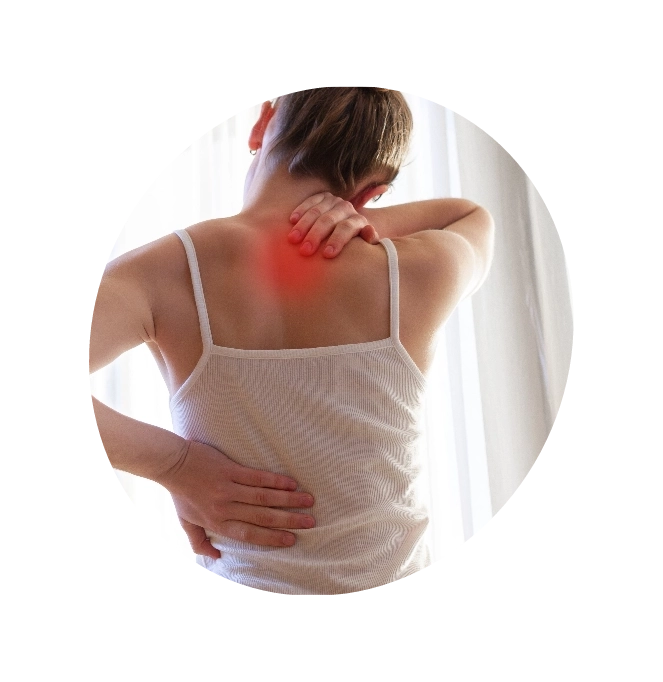
Chiropractic Care
This treatment is based on the belief that if movement in the spine is limited, then it could lead to lowered performance and aches. Spinal adjustment (manipulation) is one form of therapy chiropractors use to treat restricted spinal mobility. The goal is to restore spinal movement and, as a result, improve function and decrease pain. Chiropractors manipulate the spine from different positions using varying degrees of force. Manipulation doesn’t need to be forceful to be effective. Chiropractors can use massage and stretching to ease contracted muscles or those in spasms. This helps them to provide relief from pain, tension, and stiffness. Because manipulation has risks, always use properly trained and licensed practitioners.
Massage Therapy
Traditional healthcare methods have been around for centuries and are still being used today. It involves the use of different manipulative techniques to move your body’s muscles and soft tissues. The therapy aims to improve circulation in the muscle, increasing the flow of nutrients and eliminating waste products. Massage can reduce your heart rate, relax your muscles, improve the range of motion in your joints and increase the production of your body’s natural painkillers. It often helps relieve stress and anxiety. Although massage is usually considered a safe practice if you have any open sores, acute inflammation, or circulatory problems.
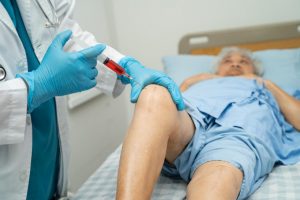
Osteopathy
Doctors of osteopathy go through rigorous and lengthy training in academic and clinical settings. They’re licensed to perform many of the same therapies and procedures as traditional doctors. Osteopathic medicine departs from the traditional forms of healing in one key aspect: the use of manipulation to resolve spinal and joint issues, similar to what chiropractic medicine does. Again, this is an area of controversy, but many studies support osteopathic techniques for many joint and muscle conditions.
Acupressure and Acupuncture
Both acupressure and acupuncture stem from the Chinese belief that 14 invisible pathways, called meridians, lie beneath your skin. In this belief, when the life force that runs through these meridians is interrupted, you become ill. Practitioners restore the flow of energy by applying pressure with their fingers (acupressure) or by inserting very fine needles (acupuncture) into the skin. There has not been definitive research to explore the potential advantages of acupressure. But according to the National Institutes of Health, acupuncture to help control pain associated with fibromyalgia may be effective.