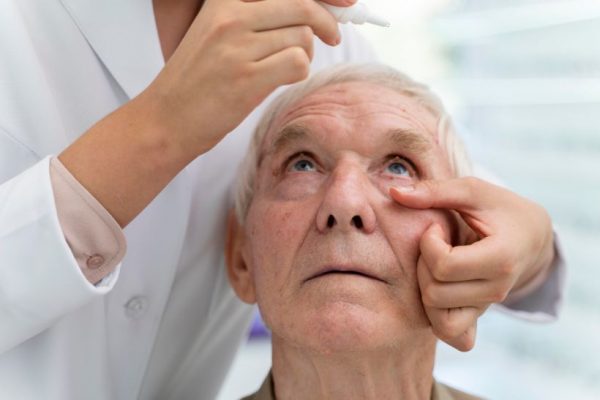
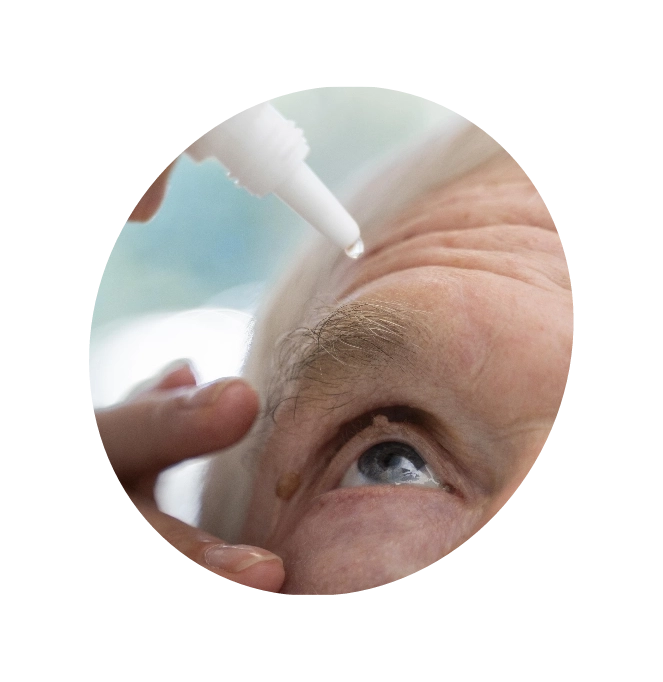
Laser
What is laser surgery? The type of laser surgery used depends on the type of glaucoma and the general health of the eye. Laser surgeries have become important in the treatment of different eye problems and medical conditions.
During the laser surgery, the eye is numbed so that there is little or no pain. The eye doctor then holds a special lens to the eye. The laser beam is aimed into the eye, and a bright light – like a camera flash – is seen.
Are there risks associated with glaucoma laser surgeries?
Laser surgery is still surgery, and can carry some risks. Some people experience a short-term increase in their intraocular pressure (IOP) soon after surgery. In others who require YAG CP (Cyclophoto-Coagulation) surgery, there is a risk of the IOP dropping too low to maintain the eye’s normal metabolism and shape. But the use of anti-glaucoma medication before and after surgery can help to reduce this risk.
The most common glaucoma laser surgeries are:
Laser Peripheral Iridotomy (LPI):
Often used in people with narrow-angle glaucoma. Narrow-angle glaucoma occurs when the angle between the iris and the cornea in the eye is too small. This causes the iris to block fluid drainage, which makes the inner eye pressure increase. LPI makes a small hole in the iris, allowing it to fall back from the fluid channel and helping the fluid drain.
Argon Laser Trabeculoplasty (ALT):
Used in people with primary open-angle glaucoma (POAG). The laser beam opens the fluid channels of the eye, helping the drainage system to work better. In many cases, medication will still be needed.
It has successfully lowered eye pressure in up to 75% of patients treated.
Selective Laser Trabeculoplasty (SLT):
Used in people with primary open-angle glaucoma (POAG). A type of laser surgery that uses a combination of frequencies allowing the laser to work at very low levels. It treats specific cells “selectively” and leaves untreated portions of the trabecular meshwork intact. For this reason, it is believed that SLT, unlike other types of laser surgery, may be safely repeated many times.
Nd:YAG Laser Cyclophoto-coagulation (YAG CP):
Used in people with severe glaucoma damage that is not being managed by standard glaucoma surgery. This surgery destroys part of the ciliary body, the part of the eye that produces intraocular fluid.
FAQs on laser surgery
Is there pain or discomfort with glaucoma laser surgery?
There is a slight stinging sensation associated with LPI and ALT. In YAG CP laser surgery, a local anesthetic is used to numb the eye. Once the eye has been numbed, there should be little or no pain and discomfort.
What are the long-term benefits of having glaucoma laser surgery? Will a repeat procedure be needed?
Glaucoma laser surgeries help to lower the IOP in the eye. The length of time the IOP is lowered depends on the type of laser surgery, the type of glaucoma, age, race, and many other factors. Some people may need the surgery repeated to get better control of the IOP, depending on the type of laser surgery done.
Is it common to have laser surgery over two sessions?
For people requiring ALT surgery, half of the fluid channels are usually treated first. Depending on the person’s eye, the other fluid channels can be treated at different times. This method prevents over-correction and lowers the risk of an increased IOP after the surgery.
Will laser surgery eliminate the need for medications?
In most cases, medications are still necessary to control and maintain eye pressure. However, surgery may lessen the amount of medication needed.
How much recovery time is needed after laser surgery?
Laser surgery is usually performed in an eye doctor’s office or eye clinic. Before the surgery, the eye will be numbed with medicine. The eye may be a bit irritated and vision may be slightly blurry after laser surgery. A ride home on the day of the surgery should be arranged.
In general, patients can resume their normal daily activities the day after the surgery. But it is important to discuss any questions or concerns about laser surgery with the eye doctor.
Does glaucoma laser surgery increase the risk of developing cataracts?
There is a small risk of developing cataracts after some types of laser surgery for glaucoma. However, the potential benefits of the surgery usually outweigh any risks.
There is a common myth that lasers can be used to remove cataracts; this is not the case except in experimental studies. After a cataract has been taken out with conventional cutting surgery, there often remains an outer membrane lens capsule. This membrane can slowly thicken and cloud vision, just as the cataract did. Laser surgery can open this membrane, helping to clear vision without an operation. This laser procedure is called a capsulotomy.
Filtering surgery
What is filtering microsurgery?
When medicines and laser surgeries do not lower eye pressure adequately, therefore doctors may recommend a procedure called filtering microsurgery (sometimes called conventional or cutting surgery).
In filtering microsurgery, a tiny drainage hole is made in the sclera (the white part of the eye) in a procedure called a trabeculectomy or a sclerostomy. The new drainage hole allows fluid to flow out of the eye and helps lower eye pressure. This prevents or reduces damage to the optic nerve.
Is there pain during the microsurgery?
In most cases, there is no pain involved. The surgery is usually done with a local anesthetic and relaxing medications. Often a limited type of anesthesia, called intravenous (I.V.) sedation, is used.
In addition, an injection is given around or behind the eye to prevent eye movement. This injection is not painful when I.V. sedation is used first. The patient will be relaxed and drowsy and will not experience any pain during surgery.
How does the eye doctor determine if filtering surgery is needed?
Often, laser surgery is recommended before filtering microsurgery, unless the eye pressure is very high or the optic nerve is badly damaged. During laser surgery, a tiny but powerful beam of light is used to make several small scars in the eye’s trabecular meshwork (the eye’s drainage system). The scars help increase the flow of fluid out of the eye.
In contrast, filtering microsurgery involves creating a drainage hole with the use of a small surgical tool. When laser surgery does not successfully lower eye pressure, or the lowering effects wear off, the doctor may recommend filtering microsurgery.
What is the success rate?
Most of the related studies document follow-up for one year. In those reports, it shows that in older patients, glaucoma filtering surgery is successful in about 70-90% of cases, for at least one year.
Occasionally, the surgically-created drainage hole begins to close and the pressure rises again. This happens because the body tries to heal the new opening in the eye as if the opening were an injury. This rapid healing occurs most often in younger people because they have a stronger healing system. Anti-wound healing drugs, such as mitomycin-C and 5-FU, help slow down the healing of the opening. If needed, glaucoma filtering surgery can be done several times in the same eye.
Is this an outpatient procedure or is an overnight stay in the hospital needed?
Usually, filtering surgery is an outpatient procedure, requiring no overnight hospital stay. Within a few days after surgery, the eye doctor will need to check on the eye pressure. The doctor will also look for any signs of infection or an increase in inflammation.
How long is the recovery time?
For at least one week after surgery, patients are advised to keep water out of the eye. Most daily activities can be done, however, it is important to avoid driving, reading, bending, and doing any heavy lifting. Since each case is different, patients should check with their doctor for specific advice.
How will the eye look after surgery? Is there a noticeable scar or redness?
The eye will be red and irritated shortly after surgery, and there may be increased eye tearing or watering. The inner eye fluid flows through the surgically-created hole and forms a small blister-like bump called a bleb. The bleb, usually located on the upper surface of the eye, is covered by the eyelid and is usually not visible.
Will vision be changed? Will glaucoma medications still need to be taken?
There may be some vision changes, such as blurred vision, for about six weeks after the surgery. After that time, vision will usually return to the same level it was before surgery.
Vision can sometimes improve after surgery in people who were previously using pilocarpine. When pilocarpine drops are no longer taken, the pupil returns to normal size, allowing more light to enter the eye.
In a few cases, the vision may be worse due to very low pressure. Cataracts or wrinkles in the macula area of the eye may develop.
In terms of vision correction, a patient’s glasses or contact lenses may need to be changed after surgery. Both gases permeable and soft contact lenses may be worn after glaucoma filtering surgery. There may be fitting problems due to the bleb. Special care is needed to avoid infection of the bleb. Contact lens users should discuss these problems with their eye doctor following surgery.